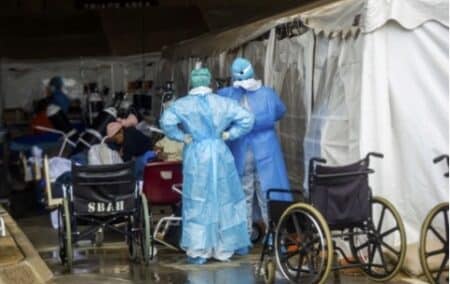
The government’s bungled and tardy Covid-19 vaccine roll-out has predictably led to an upsurge in infections, great suffering among the ill and isolated, and many hundreds of additional deaths that could have been avoided.
Yet the government declines to accept responsibility for the harm that it has done by insisting on a state monopoly over vaccine procurement. Instead, it has deployed Barry Schoub, head of the Ministerial Advisory Committee on Covid Vaccines, to castigate its critics and deny its accountability for a vaccine roll-out so slow that South Africa lags far behind almost all its peers.
However, the bungled vaccine roll-out could have one positive effect if it helps to strip away some of the myths surrounding the National Health Insurance (NHI) proposal. This could save South Africans from an even more destructive government monopoly over every single aspect of healthcare – not simply vaccine procurement.
NHI myths
SACP/ANC propaganda around the NHI repeatedly claims that public healthcare in South Africa is being crippled by a shortage of revenue and other resources. It also claims that, once the NHI has boosted available resources, public healthcare will become just as efficient as South Africa’s world-class system of private medical treatment. The NHI will thus allow the state to ‘level up’ health services so that everyone, whether rich or poor, gets the same free and high-quality care.
This perspective is flawed in at least three ways:
- health revenue is already considerable but is badly mismanaged;
- additional ‘NHI’ tax revenues may not be spent on health at all; and
- the government’s main concern is to ‘level down’ rather than ‘level up’.
Mismanagement of considerable resources
Spending on public healthcare as a percentage of GDP has already risen sharply: from 2.3% in 2002 to 4.5% in 2018, which is not far short of the 5% of GDP the World Health Organisation (WHO) recommends. In addition, the number of GPs in the public sector more than doubled between 2002 and 2020, while the number of specialists went up by close on a third.
Despite increased resources, outcomes often remain poor. Some 85% of public clinics and hospitals fail to comply with basic healthcare norms and standards, even on such essentials as hygiene and the availability of medicines. In addition, South Africa lags many developing countries on under-five mortality rates, while the state’s contingent liability for alleged medical negligence has risen sharply from R28bn in 2014 to R105bn in 2019.
Experience at one Mpumalanga public clinic – which was supposed to have been ‘strengthened’ through its participation in a NHI pilot study – highlights common shortcomings.
Interviewed by The Citizen in October 2019 on whether the pilot study had helped, patients said they ‘continued to be subjected to chronic shortages of medication, rude nursing staff, long waiting hours, and a chaotic filing system’. Many arrived as early as 5am, but nurses either ignored them or ‘ridiculed and demeaned’ them if they complained. Some had therefore given up on even trying to seek treatment.
Why this inefficiency and indifference? Cadre deployment is partially to blame, as party loyalists appointed to posts know that their political affiliations count more than their job performance. Also relevant is the Labour Relations Act of 1995 – which makes it difficult to implement dismissals – and a reluctance among many public service managers to discipline their staff.
According to the Public Service Commission or PSC (a body established under the Constitution to oversee the public service), many ‘managers are too scared of trade unions’ to punish employees for poor performance. Many decline to act even against unlawful conduct, such as blocking operating theatre doors during a hospital strike.
Most managers find it easier to pay bonuses than impose penalties. The upshot, says PSC director general Irene Mathenjwa, is that employees now take the view that ‘they should be given a good score just for coming to work’, irrespective of what they achieve during their working hours.
Corruption is another key factor and goes largely unchecked. State property in hospitals and clinics is commonly ‘stolen, hired out, or resold’, as President Cyril Ramaphosa has noted. Procurement of goods and services is deeply tainted too, with many state tenders marred by ‘false invoicing, collusion,…bribery, and over-pricing’.
Unless these deeper problems are resolved, more resources for public healthcare will not improve performance. On the contrary, expanding the public healthcare budget will simply increase the scope for incompetence, mismanagement, corruption, and theft.
‘NHI’ taxes for general spending, not health
Under the NHI, the SACP/ANC alliance plans to divert much of the roughly R250bn a year that some 18 million people now spend on the private healthcare of their choice into the coffers of the state.
Though the government declines to disclose how much the NHI will cost, the Davis Tax Committee estimated in 2017 that the new system would need R165bn in additional revenue at its start. The committee also cautioned that the NHI was ‘unlikely to be sustainable’ without sustained economic growth.
Assuming R165bn is enough (which seems unlikely), how could this sum be raised? In 2019 Intellidex estimated that this would require a 2.75% payroll tax, a 2.75% surcharge on income tax, and a 3.5 percentage point increase in the VAT rate, which would take this from 15% to a damaging18.5%.
But even if this R165bn can be raised from a population already struggling under one of the highest tax burdens in the world, the money will not necessarily be used for the NHI. In the absence of legislation ring-fencing ‘NHI’ taxes for NHI purposes – which the Treasury opposes – the extra R165bn will be paid into the National Revenue Fund, as the Constitution requires.
Once included in this common pot, ‘NHI’ revenue will be used to help fund all government spending: from public service wages and SOE bailouts to the interest bill on expanding public debt. Most of the extra ‘NHI’ taxes will go, in short, to paying cadre salaries, covering inflated prices on many BEE tenders, and otherwise oiling the patronage machine that keeps the SACP/ANC alliance in power.
The assumption that the government wants to ‘level up’
The government repeatedly implies that a key purpose of the NHI is to end the disparities between public and private healthcare and ‘level up’ by providing the same high-quality treatment to all.
Generally forgotten is a telling 2004 comment by Dr Kgosi Letlape, then president of the South African Medical Association, that the government’s underlying agenda was rather to ‘get rid of the private sector in healthcare’. Behind this objective, he added, lay the health department’s philosophy that, ‘If you can’t treat everybody, you treat nobody’.
What the SACP/ANC alliance wants, in short, is to ‘level down’, rather than up. It cares little that the NHI will diminish the healthcare services now available – for all it wants to ensure is that the little that is left is shared equally among all.
NHI propaganda claims, of course, that the new system will expand health services rather than reduce them, but this is not so. Some 20% of health professionals are already taking steps to emigrate, while another 40% could leave too. The 85% of public hospitals and clinics that fail to meet basic norms will be barred from participating in the NHI. Most tellingly, the state’s monopoly over procurement will be inefficient and often corrupt, while centralised control over all health services will destroy competition and innovation.
The vaccine roll-out demonstrates the dangers
As five health experts have recently written, South Africa should have been able to make rapid progress on Covid-19 vaccines as it already had a large childhood vaccination programme and significant experience in rolling out antiretroviral treatment to millions. Instead, the country lags well behind all others on the continent because of the government’s many ‘mis-steps’.
Having insisted on being the sole vaccine purchaser, the government then dithered and delayed in developing a strategy, negotiating with suppliers, and creating a registration system to oversee the process. It then compounded its shortcomings by discarding a million AstraZeneca doses on spurious grounds, rejecting a Novavax vaccine shown to be effective against the Beta variant, and omitting to plan for unexpected contingencies.
Above all it has failed to overcome the supply constraints that are still the key obstacle to progress – and the main reason for hundreds of avoidable deaths.
The SACP/ANC alliance nevertheless seeks to move seamlessly from the state’s botched monopoly over vaccine procurement to a comprehensive state monopoly over every aspect of healthcare in the country.
This state monopoly over health will function no better than the government’s monopoly over electricity and other essential services has done. As one anaesthetist has warned, ‘the NHI will be like Eskom, SAA and the SABC combined, except that many people will die.’
[Photo: Alet Pretorius/Gallo Images via Getty Images]