This is the second in a series of five articles in which Michael Settas will provide readers with the critically important distinction between universal health coverage (a policy objective) and the proposed National Health Insurance (a financing mechanism). He provides a high-level background to the country’s two major health assets, the private and public sectors, as well as a history of health policy since 1994 that has culminated in the contentious and now imminent National Health Insurance proposal. You can read the first article here.
South Africa’s public health system is perceived poorly by many and routinely attracts negative press coverage over its numerous failures, but it nonetheless remains a substantial and important national asset, relied upon by over 80% of citizens. Its proper functioning is critical in managing the nation’s disease burden, which serves as a foundational pillar for a productive labour force as well as improving the quality of life of citizens.
The national health budget comes from general tax revenue, with the vast majority apportioned to the provinces through the provincial equitable share and conditional grants. The equitable share makes up the majority of provincial funding and since it is unconditional funding, provinces are free to allocate this as they see fit in accordance with regional health demands and/or the mix of provider types and facilities required.
In other words, the provinces hold the constitutional mandate for the distribution of budget allocations and the management of delivery of services, whereas the national department oversees policy. The provincial management is performed across 52 District Health Authorities (DHA), employing medical and administrative staff to operate facilities such as community health centres, clinics, and hospitals. It is a decentralised structure with some centralised peripheral services, such as the National Health Laboratory Services.
Care is universally free at the point-of-service and although hospital services for higher income earners are technically billable according to a means test, this is seldom applied, resulting in virtually all public services being free of charge.
Public Health Expenditure
“The primary reason for this shortage [of doctors] is that the public health sector budget has not increased in real terms for the past 10 years. This has impacted the number of staff that can be appointed”
Former Health Minister, Zweli Mkhize, Parliamentary Q&A Session, 2019
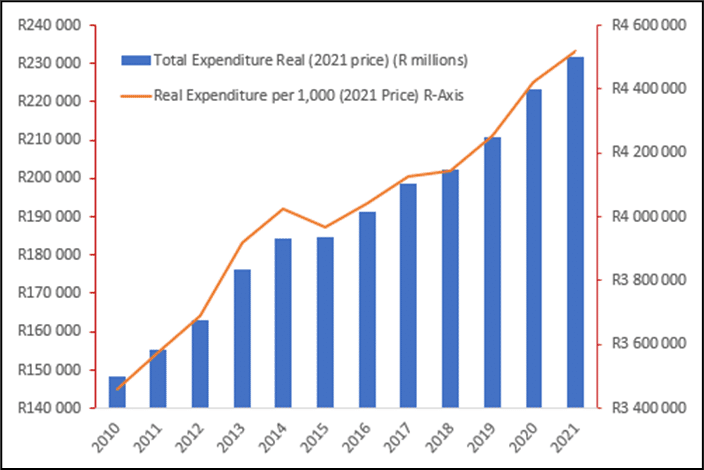
From a study covering ten years of provincial health expenditure, and by assessing the subsequent recent provincial health departments’ annual reports, one can see that provincial health expenditure grew in real terms by 49.6% from 2010 to 2021, i.e. from R148bn to R231bn in 2021 values (represented in the blue bars below).
By calculating this real expenditure per 1 000 uninsured population (i.e. those not on medical aid), one can see a real per capita increase of 25.2% from 2010 to 2021, i.e. from R3.46m to R4.51m (represented by the orange line).
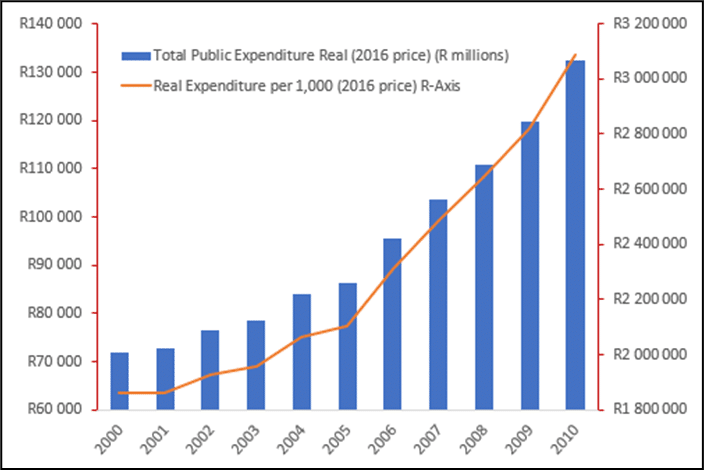
An earlier study on public health expenditure, co-authored by National Treasury, went further back in time, showing total public health expenditure from 1995 to 2016. (‘Total’ here is all sources, including National and Provincial Departments of Health, Department of Defence, Department of Correctional Services, Road Accident Fund, and Workmen’s Compensation Fund).
This shows that in the earlier decade from 2000 to 2010, public spending increased by even higher percentages than is shown above. Total expenditure grew in real terms by 84%, from R72bn in 2000 to R132bn in 2010 (2016 values are represented by the blue bars below).
Also, by measuring this against the uninsured population, one can see a real per capita health expenditure increase of 66% over this decade, i.e. from R1.86m to R3.09m per 1 000 uninsured population (2016 values are represented by the orange line in the graph below).
By any measure, public sector health expenditure has grown very substantially for the past two decades.
(Note: the public expenditure data sets used for the two graphs above differ and the price index in each is based on different years, so the two graphs are not comparable. However, the feature worth noting is the substantial upward trends in real per capita public expenditure over both periods).
International Comparison
South Africa’s public expenditure compares favourably with peer countries also classified as upper-middle income (UMI). The combined average is 4.1% of GDP, which is exactly the same as South Africa’s (2018 values).
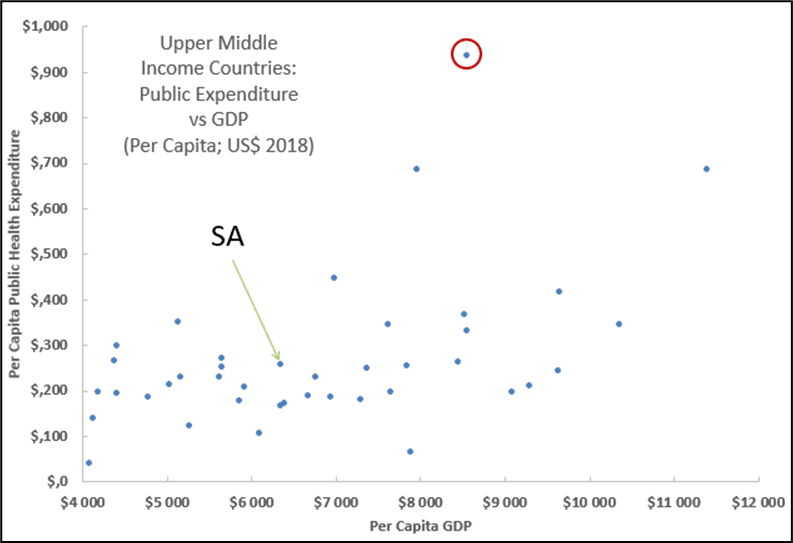
The graph below shows that, in per capita terms, a number of UMI countries with higher GDPs than South Africa spend less on public healthcare and, conversely, there are three that spend significantly more than this country.
It is, however, important to note that ‘upper-middle income’ encompasses a wide range, with the countries at the top end of the classification having a per-capita GDP close to three times that of the ones at the bottom end. As a general trend though, as GDP increases, so too does public health expenditure.
An outlier from this trend, spending more on healthcare than any UMI country at over 11% of GDP, is Cuba (circled in red in the graph below). We’ll come back to this when further examining the proposed NHI in the last article.
Public Sector Medical Personnel
The table below shows the number of medical personnel employed by the state in the major clinical disciplines from 2006 through to 2019. In all but one discipline, the ratio of medical personnel to citizens has improved, in most substantially so.
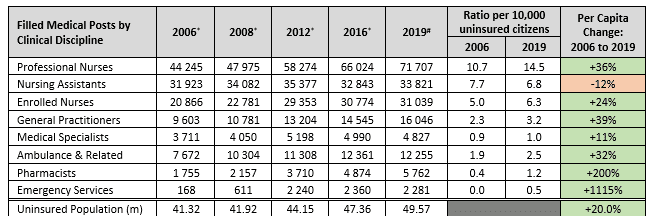
In the ten years from 2006 to 2016, the total number of medical personnel employed by the state grew by 43%, from 139 769 to 199 549. Out of 28 clinical disciplines, 22 had improvements in the ratio of medical personnel to uninsured populationduring this same period.
This is not to say that the Department of Health (DoH) is ideally resourced in personnel in every clinical discipline or that there are not regional disparities, but overall there has been very substantial growth over most disciplines for an extended time period.
In the first article I showed that the one problem statement that government is relying on to support the National Health Insurance (NHI) proposal, is that public sector financial resources have been declining, resulting in the public sector’s growing quality problems.
However, as we can see from the above, both financial and human resources have consistently and substantially increased over the past two decades, in both real and per capita terms, so this statement supporting the NHI policy simply does not stand up to scrutiny.
“This maldistribution of human resources [between the public and private sectors] is at the root of the health care crisis”
Dr Olive Shisana, Chairperson of the Ministerial Advisory Committee on NHI, 2019
If anything, health outcomes and quality of care in the public sector should have improved over this period. But this has clearly not been the case, which indicates a more systemic underlying issue, or possibly multiple issues, that are causal to the state’s problems. I examine this in more detail in a later article.
Public Hospitals
A 2019 study on public sector hospitals indicates that there are approximately 88 000 beds in over 400 hospitals, providing a ratio of 17.8 beds per 10 000 uninsured citizens. This ratio has declined from 24.0 in 2003, as population growth has outstripped investment into new hospitals.
The authors of the study considered a bed density of 18 and higher to be saturated – densities lower than this would likely be inadequate to serve their populations. Although the demand for hospital beds has declined globally in recent decades, owing to new medical technologies and methods limiting the average lengths-of-stay and admission rates, South Africa’s rapid urbanisation is causing problems in planning regional hospital capacities.
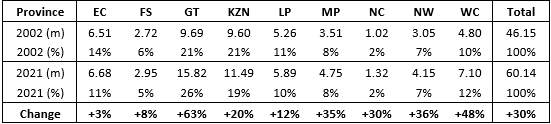
The table below shows that the total populations in South Africa’s two richest provinces – Gauteng and Western Cape – have grown by 63% and 48% respectively between 2002 and 2021. Conversely, the Eastern Cape, Free State, and Limpopo have only increased by 3%, 8% and 12% respectively over this period. This is substantially lower than the national average population growth of 30%.
These migratory shifts in population and the national growth of 30% have resulted in hospital bed densities varying substantially from region to region and declining overall at a national level. The following table shows the hospital bed densities across the 52 District Health Authorities, and we can see here that only one third of the districts have what is considered sufficient bed capacity (18+).
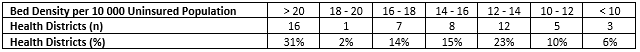
South Africa is following the global trend amongst developing economies of a declining fertility rate – in 1990 it was 3.0 whereas by 2019 it had fallen to 2.1. Nonetheless the population is still growing rapidly, with a projected national figure of over 70 million by 2040.
Proper planning with projections on population shifts will be needed to create capacity in the future. A growing population means we need more hospitals and more clinical staff to manage them, and importantly, that these facilities are built where the citizens work and live. It furthermore requires that all existing facilities are properly maintained and upgraded where required.
This leads to a discussion on a disjuncture that exists within public departments – that of infrastructure maintenance and development. The budgets for the recipient departments are allocated outside of those departments, within the Department of Public Works, which is responsible for the maintenance of existing public facilities and development of new ones. In the case of the DoH, this means it is required to engage with the Department of Public Works in planning and managing maintenance and development of new hospitals.
There is clearly substantial failure in these engagements, since there is a manifest lack of maintenance in public hospitals, which routinely record a litany of problems from malfunctioning elevators, backup electricity generators, geysers, air-conditioners, water supplies, and safety equipment.
Recent examples of these are the problems cited by suspended paediatric gastroenterologist Dr Tim de Maayer at the Rahima Moosa Mother and Child Hospital in June 2022, and the fire at Charlotte Maxeke Johannesburg Hospital in April 2021.
Dr de Maayer released an open letter to the health department – an excellent read for anyone wanting to understand a cry from the big heart of a truly committed doctor. The letter amply highlights how severe these maintenance maladies are, and the severe limitations they impose on doctors trying to ensure the best outcomes for patients.
The reaction from the Rahima Moosa hospital CEO was to suspend Dr de Maayer, with zero response to his issues raised. This is a perfect example of the often shameless and disgraceful behaviour emanating from public health officials.
“It is not like our healthcare professionals have not raised these issues multiple times through the correct channels, but nothing has happened. How much louder can our doctors and clinicians on the ground speak?”
(Prof Shabir Madhi, Dean of the Wits Faculty of Health Sciences on Dr de Maayer’s suspension.)
After the fire at the Charlotte Maxeke Johannesburg Hospital in April 2021, Spotlight released the statement below in an article after they had discussions with the fire fighters. Also bear in mind that a safety compliance audit for the hospital had been signed off just prior to the fire:
“Two senior firefighters from the City of Johannesburg who spoke to Spotlight say the two failings mentioned by Kekana above alone would sink a basic inspection or compliance audit. It was also not just the fire doors and the hydrant couplings that were faulty at Charlotte Maxeke. They say firefighters were not given building and floor plans of the hospital’s emergency exit plan when they arrived on the scene the day of the fire on April 16. The emergency exit plan is essential for those needing to enter a burning building. Smoke detection systems, fire alarms, sprinkler systems, and the mechanisms that would have triggered the magnetic smoke doors were also not in working condition. There was also water flow and low pressure to the hydrants besides non-compatible hose couplings.”
By all accounts available, public hospitals are often in a mess or vulnerable to damage because maintenance is simply absent or of insufficient quality.
What Now?
When I discuss the growth in resources with public sector doctors, mostly caring and committed individuals like Dr de Maayer, they almost always shake their heads in disbelief. And this is because it simply does not reflect their lived experiences of working within the public sector.
Besides the issue of maintenance at hospitals, another well-known phenomenon amongst the public sector workforce is the abuse of the remunerative-work-outside-public-service (RWOPS) allowance. Public-sector personnel are permitted to undertake RWOPS to a limited extent. It appears, however, that the enabling of this limited allowance has led to widespread ‘moonlighting’ – a practice where public-sector staff undertake extensive periods of paid work outside of the public sector, while maintaining their official paid public sector positions. A 2014 survey by Laetitia Rispel, Professor of Public Health at the University of the Witwatersrand, showed that amongst nursing staff this practice is highly prevalent (±40% of nurses).
Indications are that this practice is also widespread amongst other provider disciplines, making it a plausible explanation of why staff shortages remain evident in the public sector, even though the official number of staff employed has grown substantially. There are also counter arguments that RWOPS remains a ‘necessary evil’ that requires better management from the DoH. Nonetheless, there is enough evidence that moonlighting is a significant issue, yet there appears to be very little response from government on how to remedy this situation, demonstrating another failure in leadership and accountability from the health department.
Nonetheless, in principle the RWOPS allowance is a policy contradiction for the NHI proposal, which blames an oversupply of private sector resources for the state’s inability to provide adequate quality healthcare. If this is true, why permit the RWOPS policy in the first instance, if it undermines the state’s capacity and further serves to oversupply the private sector?
Any person reading this article must conclude that there is a disconnect between the growth in available resources in the public health sector and the trajectory of outcomes. Even if the conclusion is that South Africa does not have sufficient resources to provide a comprehensive basket of public care (which is probable), there should at the very least have been notable improvements in the quality and outcomes over the past 15 years, rather than the dramatic deterioration that is becoming so evident on an almost daily basis.
These facts point towards there being a systemic lack of governance and proper management of facilities, which will be covered in the next article, where I examine public sector outcomes as well as the state’s burgeoning medicolegal liability.
The views of the writer are not necessarily the views of the Daily Friend or the IRR
If you like what you have just read, support the Daily Friend